As a pediatric pelvic health therapist, you often sit at the intersection between what families report, what kids experience, and what the medical records show. More often than not, those three things don’t perfectly line up.
You may have a child who stools daily but still struggles with bladder symptoms. Or a child whose constipation is described as “well managed,” yet progress in therapy feels stalled. This is where additional investigative tools can be invaluable. Imaging is not meant to replace clinical reasoning, but to sharpen it.

One of those investigative tools is the KUB x-ray (Kidneys, Ureters, Bladder). While it’s not a standard x-ray ordered for every constipated child, it is commonly used in pediatric gastrointestinal and urology clinics. For therapists who understand how to ask for the right information and how to interpret the findings, a KUB can provide critical insight into bowel status and help guide the child’s care recommendations.
Let’s dive into this.
When A KUB X-ray Is Appropriate
A KUB is a non-invasive abdominal x-ray that allows visualization of stool throughout the colon and rectum. It’s not necessary or appropriate to order a KUB for every child with constipation. Many kids can be managed successfully based on history, symptom patterns, and response to intervention alone.
However, a KUB can help identify underlying fecal retention that isn’t obvious from bowel frequency alone. These are more often ordered in specialty settings or in cases where symptoms persist despite “doing all the right things”. This is particularly important for children with bladder dysfunction, recurrent UTIs, vesicoureteral reflux, or complex bowel and bladder issues.
Understanding when imaging adds value is part of developing clinical maturity as a pediatric pelvic health therapist. Learning how to collaborate effectively with medical providers is essential as well.

What Radiologists Are Actually Looking For
One of the biggest gaps between therapists and imaging is not what a KUB can show, but what actually gets reported.
Radiologists are capable of providing information that is extremely useful for pelvic health clinicians. Sometimes, however, unless the radiologist is prompted, those details may not make it into the final report.
Two findings are especially important.
Stool Burden
Radiologists can categorize stool burden as mild, moderate, or severe. But this language is often omitted unless specifically requested. Instead, reports may include vague phrasing that doesn’t clearly communicate clinical significance.
For a therapist trying to determine whether bowel management needs to be escalated, that lack of specificity can be frustrating.
Rectal Diameter
A larger than normal rectal diameter is indicative of rectal distention and fecal retention.
Rectal distention has significant implications for interoception and bowel emptying patterns, yet this measurement is frequently left out of reports.
Remember, though, that you cannot make this measurement yourself by visually estimating the image. Rectal diameter must be measured using the imaging equipment at the time the image is taken, and formally documented by the radiologist.
Recent research actually does not support the use of KUB’s for constipation. Ultrasound is recommended for assessing fecal impaction. In most bowel management programs KUB’s are still routinely used to assess the stool in the entire colon.
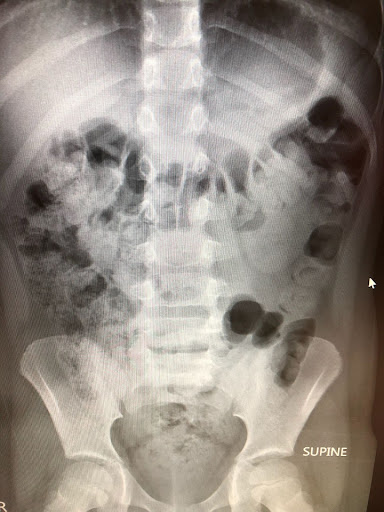
Asking Better Questions As A Therapist
Advocacy is a skill, and this is one place where it truly matters.
When collaborating with referring providers or specialty clinics, you should feel confident requesting that the radiology report specifically comment on the stool burden. Not all radiologists measure rectal diameter but it is fairly easy to assess visually, especially when the stool fills the entire pelvic rim.
This isn’t about stepping outside your scope. You want to ensure that the imaging provides information that meaningfully supports your treatment interventions.
Furthermore, reading the radiology report alone often isn’t enough. Looking at the actual images can provide important context, especially when the written findings don’t align with the child’s symptoms or functional presentation. Stool distribution and rectal size can be visually striking, even when the report language feels understated. I always ask to see a picture of the x-ray myself.
This doesn’t mean you should interpret imaging independently or diagnose from x-rays. It means you should be able to understand what you’re seeing well enough to integrate it into your broader clinical picture.

Learning how to communicate your needs clearly with other providers is something many therapists don’t get taught formally, which is why this type of interdisciplinary reasoning is emphasized throughout my online course Pediatrics Level 1–Treatment of Bowel and Bladder Disorders.
Cleanouts And The Reality Of Residual Stool
A common misconception that parents, and even many providers, have is that completing a cleanout means the bowel is “clear.”
In reality, children can complete a cleanout and still show significant stool burden on a follow-up KUB. This happens frequently.
Liquid stool output does not automatically indicate effective evacuation. If the stool looks like chocolate pudding, the child is not fully cleaned out. The stool should look like lemonade.
In fact, I once worked with a child who required three cleanouts, spaced one week apart with hydration time in between, before imaging confirmed that she was fully cleared. Until then, symptoms persisted despite what appeared to be adequate intervention.
A kid can have a bowel movement every day with a soft stool, yet still have significant fecal retention. In fact, 47% of children who present like this ARE constipated!
This is why I often tell families, “You’re constipated until proven innocent.”
Bowel frequency alone is not a reliable indicator of bowel health. Always ask about straining with bowel movements.
Chronic impaction affects far more than stooling patterns. It can impair nutrient absorption, alter gut motility, and disrupt the microbiome. When the bowel is mechanically overloaded, the system cannot function optimally, regardless of how “normal” things look on the surface.
Case Example: The Seven-Year-Old Who Was “Well Managed”
A powerful example of this comes from a seven-year-old girl I worked with who had a history of vesicoureteral reflux. Constipation was noted in her medical history, but it was considered “well managed”.
She took MiraLax (PEG) and had a bowel movement daily. She produced soft stool of Type 4 on the Bristol scale.. So no obvious red flags. From a symptom standpoint, there was little reason for concern.

However, when she returned to her pediatric urologist, a KUB was ordered as part of routine follow-up. The imaging revealed calcified stool in the transverse colon.
Despite appropriate medication use and regular bowel movements, stool had become caked onto the bowel wall, effectively narrowing the lumen. In other words, the pipe had become smaller from the inside.
This finding significantly changed how her care was approached and highlighted how easily retained stool can be missed without imaging.
Using KUBs To Direct–Not Dictate–Care
KUB x-rays don’t replace your assessment skills. Nor do they tell you which exercises to prescribe or how to cue coordination.
What they do provide is objective data that can support your clinical decision making, help educate families, and set realistic expectations for your patient’s progress.
Knowing when to request imaging, how to interpret the findings, and how to integrate that information into conservative care can elevate your confidence as a pediatric pelvic health therapist.
Fun Fact- ask if the radiology department uses a pediatric protocol which delivers less radiation than adult protocols!
In my online course, Peds Level 1–Treatment of Bowel and Bladder Disorders, KUB imaging is discussed alongside other investigative tools. You also learn about comprehensive history taking, bowel and bladder assessment, and patient/parent education. Imaging without context is incomplete, and context without data can leave important gaps.
You’re not just treating what the child reports. You are directing care with intention and evidence. That is what makes a real difference for your patients and for their families.
